What Is Fasting Insulin?
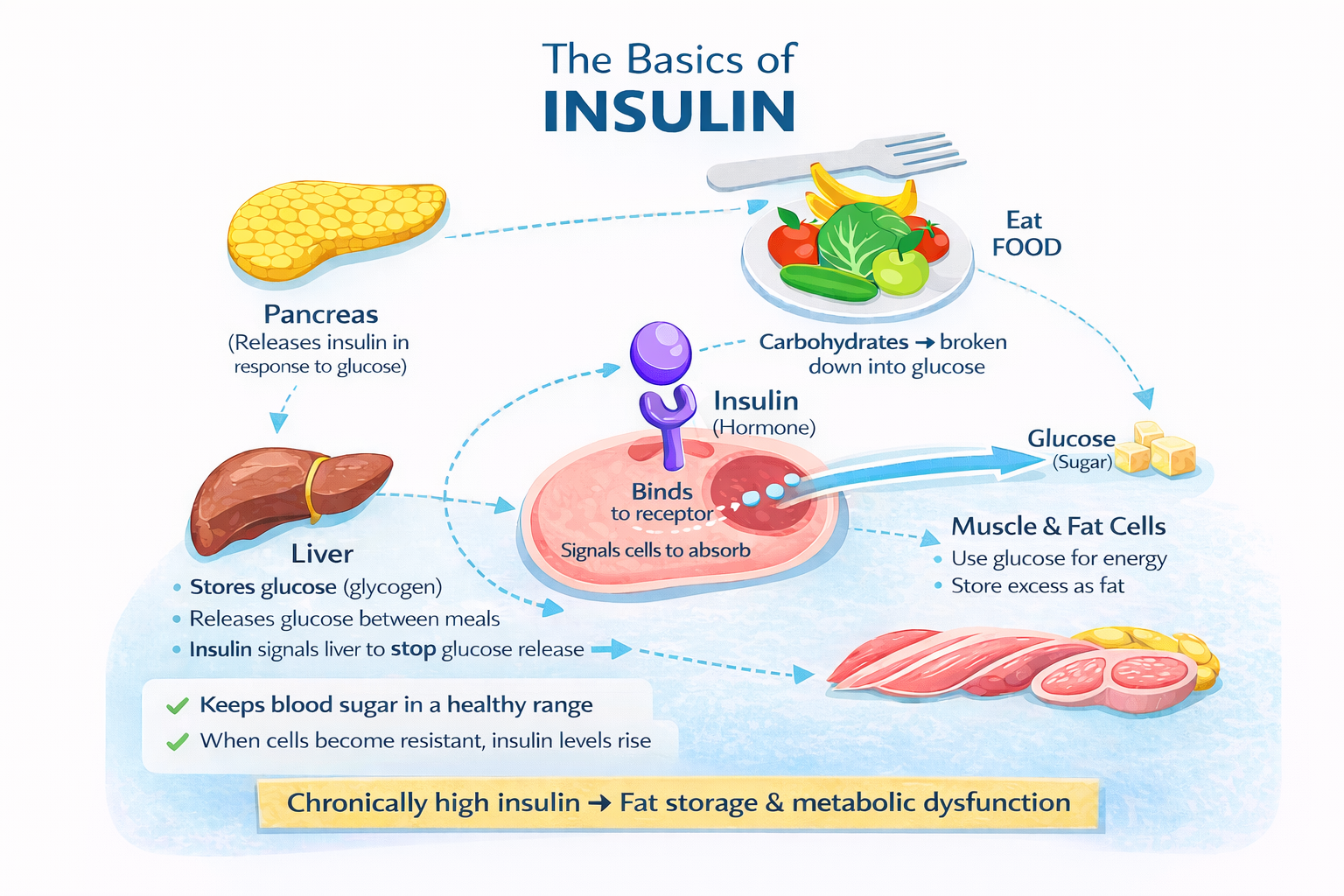
Fasting insulin is a blood test that measures how much insulin your body is producing to keep blood sugar stable. It’s one of the earliest indicators of metabolic dysfunction and insulin resistance.
Key Takeaways
- Fasting insulin can detect blood sugar issues earlier than A1C
- “Normal” lab ranges are often too broad to catch early dysfunction
- Elevated insulin is linked to weight gain, fatigue, and high cholesterol
- Most conventional doctors don’t routinely test it
- Improving fasting insulin is possible with targeted nutrition and lifestyle strategies
What Is a Healthy Fasting Insulin Level?
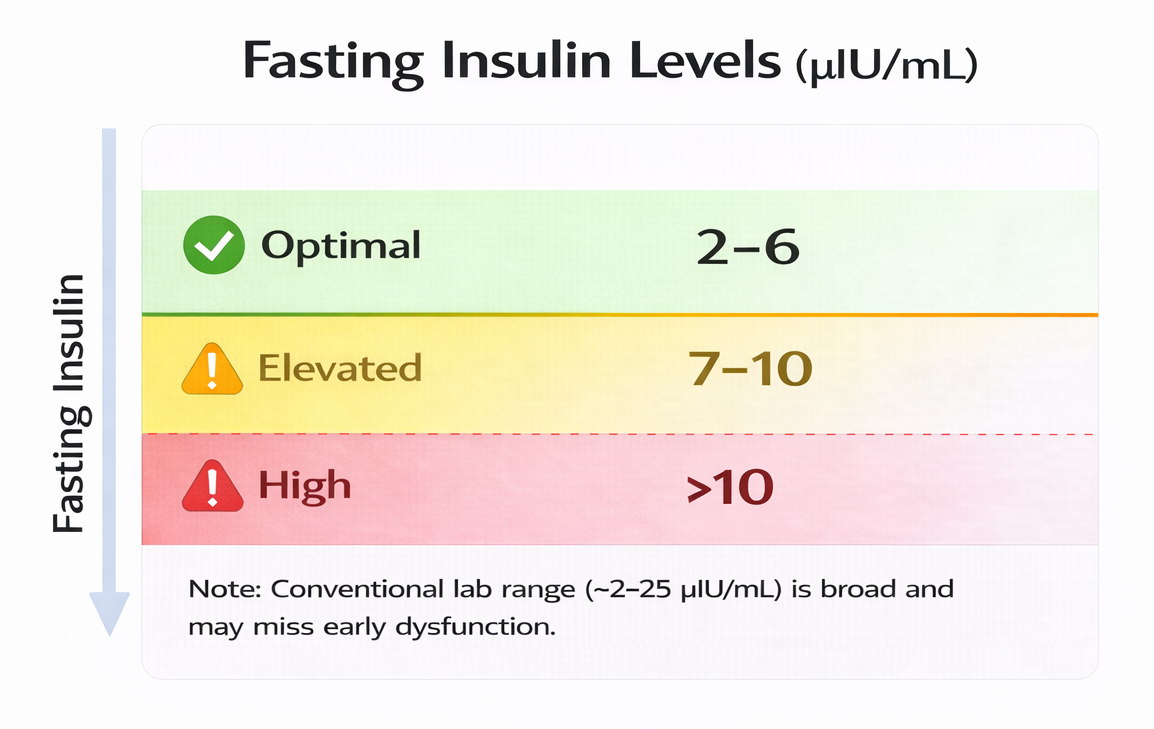
Most standard lab ranges consider fasting insulin “normal” anywhere from about 2 to 25 µIU/mL.
From a functional and metabolic health perspective:
- Optimal: ~2–6 µIU/mL
- Moderately elevated: 7–10 µIU/mL
- High (insulin resistance likely): >10 µIU/mL
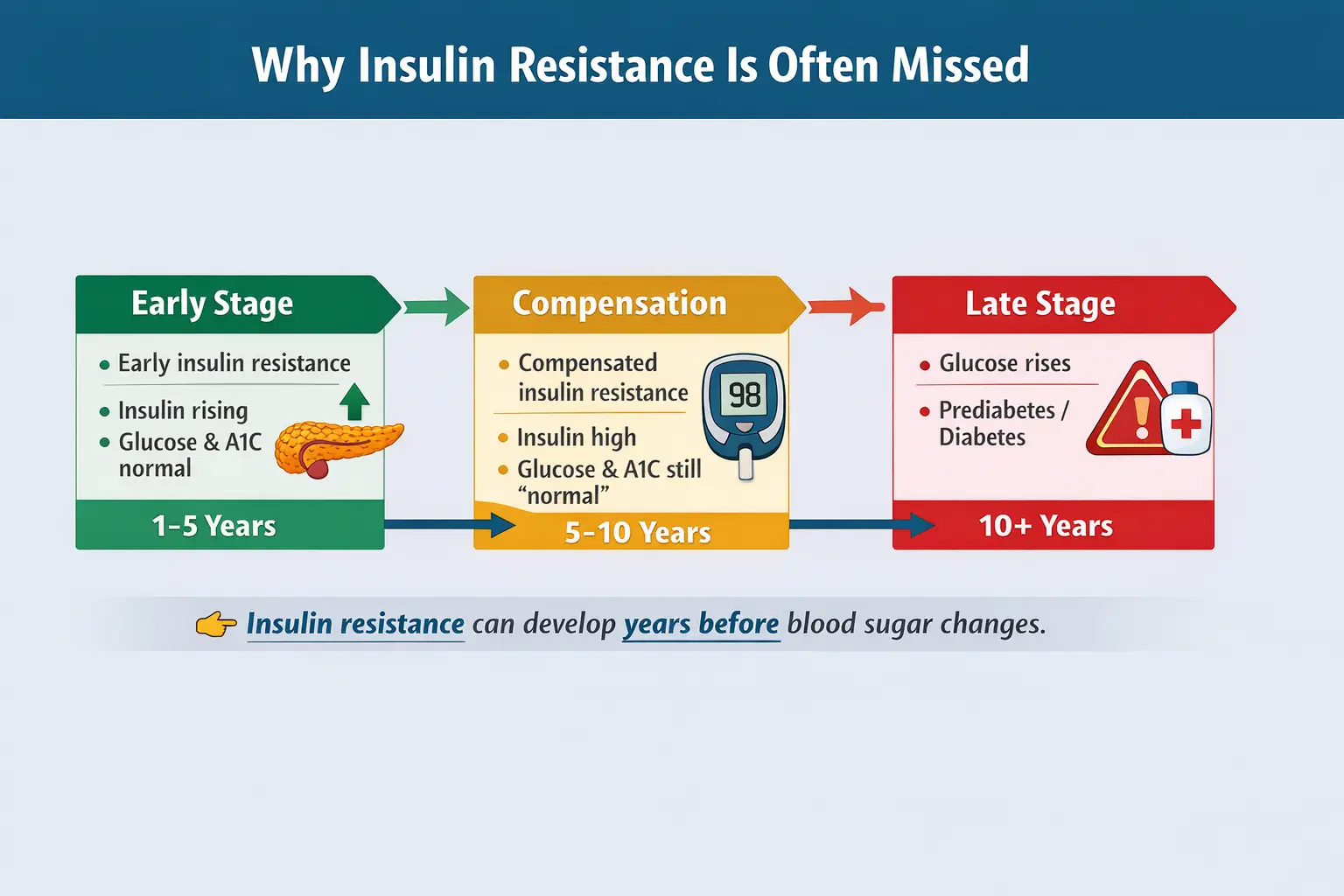
 Why Your Doctor Might Not Be Testing It
Why Your Doctor Might Not Be Testing It
Fasting insulin is not typically included in routine blood work.
Most doctors rely on fasting glucose and A1C, which often don’t change until blood sugar has been struggling for years.
Your body compensates by producing more insulin to keep glucose levels “normal.” On paper, everything looks fine, while your metabolism is working overtime.
So you get told:
👉 “Your labs look fine.”
Meanwhile:
- Insulin is rising
- Fat storage is increasing
- Energy is declining
- Metabolic dysfunction is progressing
This gets missed because:
- The system is designed to catch disease, not early dysfunction
- Clinical guidelines evolve slowly
- Fasting insulin isn’t part of standard lab panels
- “Normal” doesn’t mean optimal
The result? A lot of people are told they’re “fine” right up until they’re not. Insulin resistance is a key driver of metabolic dysfunction and often develops long before blood sugar levels rise.
If you want a clearer picture of your metabolic health beyond standard labs, functional lab testing can help uncover early imbalances that are often missed.
Insulin Resistance Timeline
Why Fasting Insulin Matters for Your Health
High fasting insulin is associated with:
- Weight gain, especially around the midsection
- Difficulty losing weight despite eating well
- Increased triglycerides
- Lower HDL cholesterol
- Increased risk for prediabetes and type 2 diabetes
- Hormonal imbalances
Signs Your Insulin May Be Elevated
- Cravings for sugar or carbs
- Energy crashes, especially in the afternoon
- Feeling shaky or irritable when you haven’t eaten
- Stubborn weight, particularly abdominal fat
- Brain fog or fatigue after meals
How to Improve Fasting Insulin Naturally
- Balance your meals with protein, fiber, and healthy fats
Helps stabilize blood sugar and reduce insulin spikes - Be strategic with carbohydrates
Avoid eating carbs alone to support better glucose control - Build muscle through strength training
Improves insulin sensitivity and glucose uptake, particularly in skeletal muscle (See research supporting this.) - Prioritize sleep quality
Poor sleep can negatively impact metabolism and increase sugar cravings - Manage stress
Chronic stress can increase insulin and drive metabolic dysfunction - Optimize gut health
Digestive issues like bloating, constipation, or diarrhea may contribute to insulin resistance and metabolic dysfunction
The Bottom Line
Fasting insulin is one of the most valuable and underutilized markers for understanding your metabolic health. Catching elevated insulin early gives you the opportunity to prevent progression to prediabetes and improve energy and metabolism.
Want a More Personalized Approach?
If your labs are “normal” but you don’t feel your best, there’s often underlying metabolic dysfunction beneath the surface.
My Metabolic Shift Strategy™ takes a deeper, root-cause approach using advanced lab testing, personalized nutrition, and targeted lifestyle strategies.
👉 Learn more about the METABOLIC SHIFT STRATEGY.™
👉 Start your 1:1 plan here: BOOK YOUR FREE STRATEGY CALL
Written by Ana Coyle, MS, RDN, IFMCP
Functional Dietitian specializing in metabolic health and root-cause nutrition.